Oral Thrush: Symptoms, Causes, Treatment & How to Get Rid of It
Oral thrush is a common fungal infection that affects the mouth and surrounding tissues.
It occurs when a naturally present fungus, Candida, overgrows and disrupts the normal balance of microorganisms in the oral cavity.
Although it is usually mild, oral thrush can become persistent or severe in certain individuals, especially when underlying risk factors are present.
👉 It is not just an infection; it is often a signal of imbalance in the oral or immune system.
What Is Oral Thrush?
Oral thrush, also known as oral candidiasis, is an infection caused by the overgrowth of Candida species, most commonly Candida albicans.
This microorganism normally exists in small amounts in the mouth without causing harm. However, when conditions favor its growth, it can multiply rapidly and lead to visible and symptomatic infection.
The result is a characteristic appearance of white lesions in the mouth, often accompanied by discomfort or altered taste.
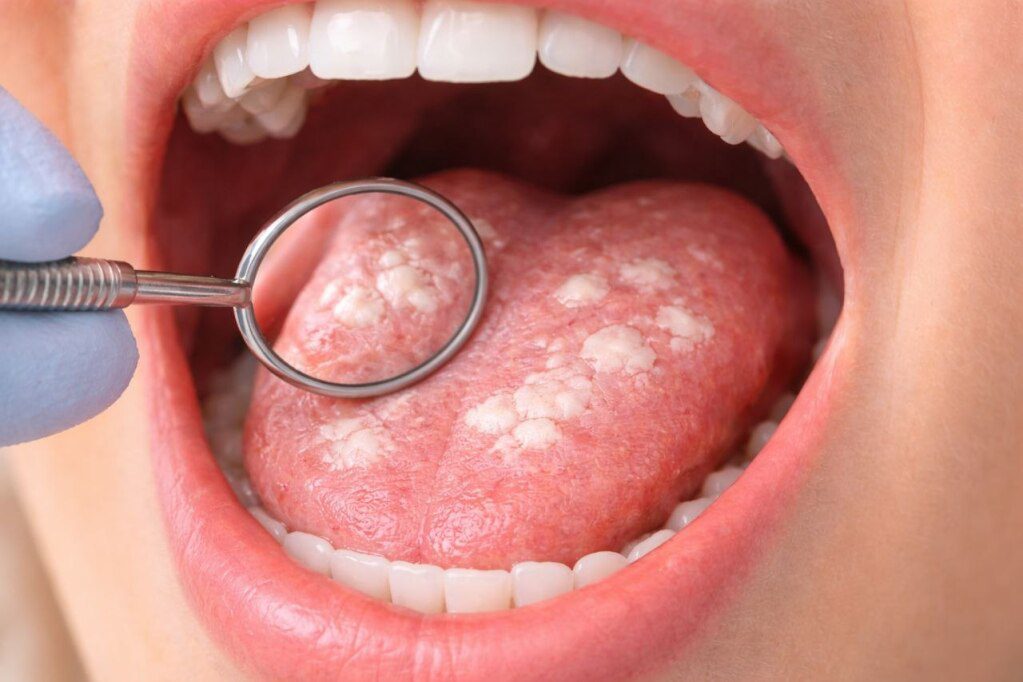
What Does Oral Thrush Look Like?
The most recognizable feature of oral thrush is the presence of creamy white patches on the tongue, inner cheeks, gums, or palate.
These patches may look similar to milk residue, but, unlike normal debris, they cannot be easily wiped away without causing irritation or slight bleeding.
In some cases, the underlying tissue appears red and inflamed, especially if the white coating is removed.
Symptoms of Oral Thrush
Symptoms can vary depending on severity and the individual’s overall health.
In mild cases, the condition may cause little discomfort beyond the visible lesions.
As it progresses, patients may experience a burning sensation, difficulty swallowing, or a persistent unpleasant taste. Some describe a cotton-like feeling in the mouth.
In more advanced cases, cracking at the corners of the mouth (angular cheilitis) or spreading of the infection toward the throat can occur.
Why Oral Thrush Develops
Oral thrush is not simply the presence of fungus; it is the result of an imbalance in the oral ecosystem.
Under normal conditions, bacteria and the immune system keep Candida growth under control.
When this balance is disrupted, the fungus can overgrow and cause infection.
🔹Common Triggers
- Antibiotic use is one of the most frequent causes, as it reduces the bacterial population that normally limits fungal growth.
- A weakened immune system also plays a major role, making individuals more susceptible to infection.
- Other contributing factors include dry mouth, poorly controlled diabetes, smoking, and the use of dentures, especially if they are not cleaned properly.
Who Is at Higher Risk?
While oral thrush can affect anyone, it is more common in specific groups.
Infants are particularly susceptible because their immune systems are still developing.
Older adults, especially those who wear dentures, are also at increased risk.
Individuals with compromised immunity, such as those undergoing medical treatments or living with chronic conditions, are more likely to experience persistent or recurrent infections.
How Oral Thrush Is Diagnosed
Diagnosis is usually straightforward and based on clinical examination.
The appearance of the lesions, combined with patient history, is often sufficient for identification.
In uncertain cases, a sample may be taken and analyzed to confirm the presence of fungal organisms.
Treatment of Oral Thrush
Treatment focuses on eliminating the fungal overgrowth while addressing the underlying cause.
🔹Antifungal Medications
The most common approach involves antifungal agents, which may be prescribed as mouth rinses, lozenges, or systemic medications depending on severity.
These treatments work by inhibiting fungal growth and restoring balance in the oral microbiome.
🔹Addressing Underlying Factors
Treating oral thrush effectively requires more than just medication.
If the infection is related to antibiotic use, dry mouth, or poorly controlled diabetes, these factors must be managed to prevent recurrence.
For denture wearers, proper hygiene is essential to eliminate fungal reservoirs.
Can Oral Thrush Go Away on Its Own?
In some mild cases, especially in otherwise healthy individuals, oral thrush may resolve without treatment.
However, relying on spontaneous resolution is not recommended, particularly if symptoms persist or worsen.
👉 Persistent thrush often indicates an underlying issue that needs attention.
How to Prevent Oral Thrush
Prevention is largely about maintaining balance in the oral environment.
Good oral hygiene plays a central role, including regular brushing and cleaning of dentures if present.
Limiting unnecessary antibiotic use, when possible, helps preserve the natural microbial balance.
Managing systemic conditions such as diabetes and staying hydrated to support saliva production are also important protective factors.
Is Oral Thrush Contagious?
Oral thrush is not typically considered highly contagious in healthy individuals.
However, it can be transmitted under certain conditions, particularly between a mother and infant during breastfeeding or among individuals with weakened immune systems.
Clinical Insight
Oral thrush is often underestimated because it appears simple on the surface.
But clinically, it can be a marker of systemic imbalance, especially when recurrent or persistent.
👉 Treating the infection without addressing the underlying cause often leads to recurrence.
When to See a Dentist or Doctor
Professional evaluation is recommended if:
- White patches persist beyond a few days
- Pain or difficulty swallowing develops
- The infection recurs frequently
Early treatment not only resolves symptoms faster but also helps identify potential underlying conditions.
Conclusion
Oral thrush is a common but clinically meaningful infection caused by fungal overgrowth in the mouth.
While often mild, it reflects an imbalance that should not be ignored.
The key points are clear:
- It is caused by the overgrowth of Candida
- It presents with characteristic white lesions
- It is usually treatable with antifungal therapy
👉 Long-term control depends on addressing the underlying factors, not just the infection itself.
Frequently Asked Questions
What is the main cause of oral thrush?
An overgrowth of Candida, often triggered by antibiotics, weakened immunity, or dry mouth.
How do you get rid of oral thrush fast?
Antifungal medications combined with good oral hygiene are the most effective approach.
Is oral thrush painful?
It can cause discomfort or burning, especially in more advanced cases.
Can oral thrush come back?
Yes, especially if underlying risk factors are not addressed.
Is oral thrush serious?
It is usually mild, but it can indicate underlying health issues if recurrent or persistent.
References
Akpan, A., & Morgan, R. (2002). Oral candidiasis. Postgraduate Medical Journal, 78(922), 455–459. https://doi.org/10.1136/pmj.78.922.455
Williams, D., & Lewis, M. (2011). Pathogenesis and treatment of oral candidosis. Journal of Oral Microbiology, 3, 5771. https://doi.org/10.3402/jom.v3i0.5771
Samaranayake, L. P. (2009). Essential microbiology for dentistry (4th ed.). Churchill Livingstone.
